Digital health monitoring devices collect data from wearables, sensors, and connected equipment to enable real-time tracking and secure transmission. They support patient engagement and clinician insights while emphasizing privacy and accessibility. Sensor selection must balance data fidelity, comfort, and battery life to sustain use. Integration with care workflows and validated accuracy are essential for meaningful, outcome-driven care across real-world settings, prompting questions about implementation, protection, and long-term value.
How Digital Health Monitoring Works and Why It Matters
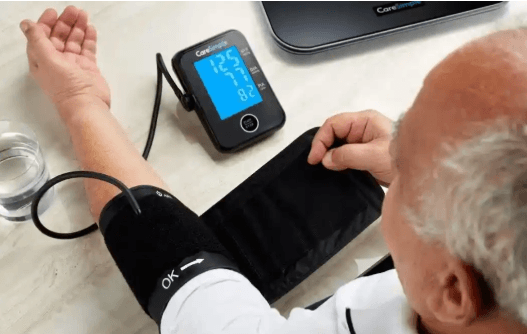
Digital health monitoring systems collect physiological data from wearable devices, sensors, and connected medical equipment to track health metrics in real time.
They translate signals into actionable insights through measurement, analytics, and secure transmission.
This supports patient engagement, clinician insights, and informed decision making, emphasizing data privacy, accessibility, and device integration.
Effective sensor selection and monitoring devices optimize health goals and overall care.
Choosing the Right Sensors for Your Health Goals
To tailor health-monitoring outcomes, it is important to select sensors aligned with specific goals and clinical contexts. Sensor choice hinges on target metrics, device interoperability, and user routine. Emphasize sensor selection that balances data fidelity with comfort and wearability. Consider battery life implications for daily use, maintenance, and reliability, ensuring sustained monitoring without frequent recharging.
Data Privacy, Accuracy, and Accessibility: What to Watch For
Data privacy, accuracy, and accessibility are key determinants of trust and usability in health-monitoring devices, shaping how data are collected, stored, and shared while influencing clinical reliability.
The discussion emphasizes data ownership, robust security standards, and consent management, ensuring transparent data flows, verifiable accuracy, and accessible interfaces while maintaining rigorous privacy protections and user autonomy in evolving digital health ecosystems.
Integrating Devices Into Care: From Wearables to Clinician Insights
Wearable devices and other patient-generated data streams increasingly feed into clinical workflows, enabling continuous monitoring, early warning signals, and more personalized care plans. The integration emphasizes wearable validation to ensure accuracy and reliability. Clinician workflow integration aligns data with existing practices, supporting decision-making without disruption. Transparent data provenance, interoperability, and secure sharing underpin scalable, outcome-driven care in real-world settings.
See also: Digital Evolution: Are We Keeping Up With Innovation?
Frequently Asked Questions
How Do I Interpret Sensor Readings for Daily Health Decisions?
Interpreting sensor readings requires cautious thresholds, recognizing interpretation pitfalls, and balancing fluctuations with trends; it emphasizes evidence-based decisions, user engagement, and data context. The detached observer notes variability, promotes corroboration, and encourages informed autonomy in daily health choices.
What Are the Hidden Costs of Long-Term Device Use?
On average, users report 12% more engagement after three months, but hidden costs emerge with long term use: maintenance, data subscriptions, and device obsolescence. Interpretation readings thus influence daily decisions while pursuing tech-enabled, freedom-focused health autonomy.
Can Devices Replace Routine Clinical Exams or Tests?
Devices cannot fully replace routine clinical exams or tests; best practice supports integration rather than substitution, acknowledging a replacement debate. They augment, not supplant, professional assessment, preventing clinical dependence while preserving patient autonomy and evidence-based decision making.
How Do I Troubleshoot Alarming Battery Drain or Connectivity Issues?
A notable 72% of users report battery anxiety; troubleshooting battery and connectivity issues begins with verifying device compatibility, updating firmware, and re-pairing. It emphasizes methodical steps for reliable performance, aligning with an evidence-based, tech-focused, freedom-seeking audience.
Are There Risks of Data Bias Affecting Personalized Insights?
Data bias can distort personalized insights, producing skewed recommendations. Rigorous validation, diverse datasets, and transparent methodology are essential to ensure accuracy. Users should seek platforms with explainable models, continuous auditing, and clear disclosures to preserve autonomy and trust.
Conclusion
Digital health monitoring devices stand at the crossroads of patient empowerment and clinical insight. Like a compass guiding ships through fog, sensors translate physiology into actionable signals. When data privacy, accuracy, and accessibility align, workflows become smoother, interventions timelier, and outcomes more predictable. The future hinges on thoughtful sensor selection, robust security, and seamless integration, echoing a quiet confidence: technology serves people best when it respects boundaries, proves its measurements, and supports clinicians in real-time decision-making.